Sleep apnea affects an estimated 50 million Americans, and roughly 80 percent of them do not know they have it. That gap between prevalence and awareness has always been concerning. A major new study has made it significantly more so. Research analyzing electronic health records from more than 11 million patients over a 23-year period has found that people with untreated sleep apnea face nearly double the risk of developing Parkinson’s disease compared to those who receive treatment. The findings, drawn from one of the most comprehensive datasets ever applied to this question, suggest that what happens during sleep may have profound consequences for the brain decades later.
Sleep apnea affects people across every demographic. It is not limited to older adults, men, people with obesity, or any other single group. The condition does not discriminate, and neither, the data suggests, does its impact on neurological health.
What sleep apnea actually does to the brain
Sleep apnea is characterized by repeated interruptions in breathing throughout the night. Each time breathing stops, oxygen levels in the body drop, and the brain is temporarily deprived of the supply it needs to function properly. A single interruption might seem insignificant. But these episodes can occur hundreds of times each night, and when multiplied across months and years, the cumulative effect on brain tissue becomes substantial.
Researchers found that the connection between untreated sleep apnea and elevated Parkinson’s risk held even after accounting for other contributing factors including age, obesity, and high blood pressure. That finding matters because it suggests the relationship between the sleep disorder and neurological decline is not simply a byproduct of other health conditions. The oxygen deprivation itself appears to play a meaningful and independent role.
How treatment changes the picture for sleep apnea patients
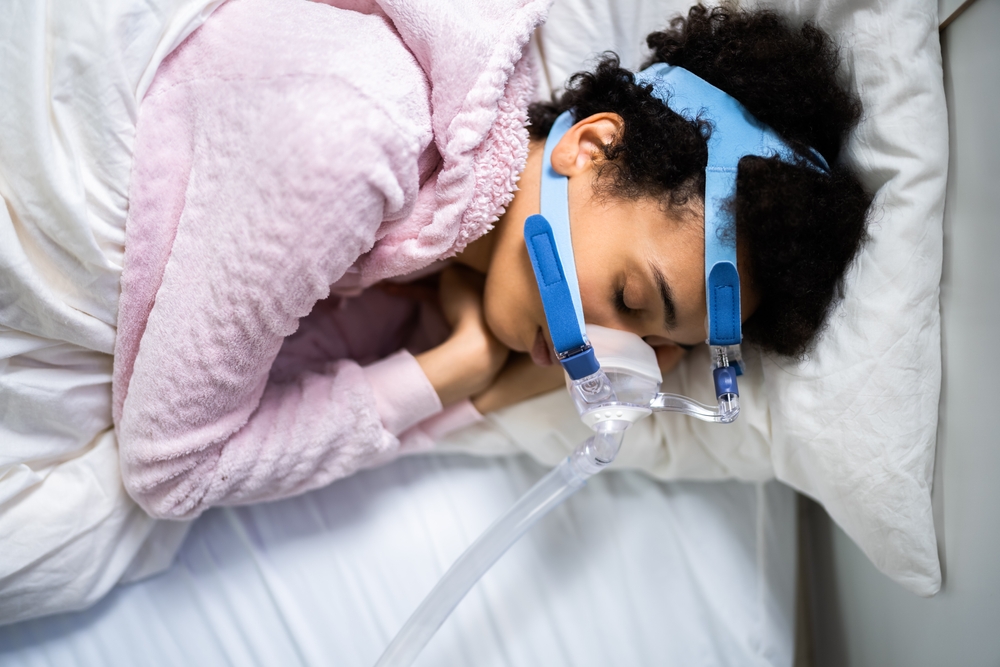
The study did not only document risk. It also identified a clear path toward reducing it. People who consistently used a CPAP machine, a device that delivers continuous air pressure to keep the airway open during sleep, showed significantly lower rates of Parkinson’s disease than those who left their condition untreated. That finding positions sleep apnea as what researchers describe as a modifiable midlife risk factor, meaning the outcome is not fixed and the decision to treat carries real long-term consequences for brain health.
CPAP therapy requires an adjustment period, and some people find the masks uncomfortable initially. The evidence from this study adds considerable weight to the argument for persistence. The discomfort of adaptation is finite. The neurological protection that consistent use appears to offer extends across decades.
Recognizing sleep apnea and knowing when to act
The most common warning signs of sleep apnea include loud or chronic snoring, waking during the night with a gasping sensation, and excessive fatigue during the day despite a full night in bed. Partners of people with sleep apnea frequently notice breathing pauses that the person themselves is unaware of. Any of these symptoms warrants a conversation with a doctor and, in most cases, a formal sleep study.
One of the more persistent misconceptions about sleep apnea is that it primarily affects a specific type of person. The reality is that it develops across all ages, body types, and genders. Feeling young, fit, or healthy is not a reliable indicator of low risk, and waiting for symptoms to become obvious may mean allowing years of unaddressed neurological impact.
The quality of sleep happening each night is shaping the health of the brain over the long term. Treating sleep apnea is not simply about feeling more rested. It is about protecting the neurons that determine how the brain functions years and decades from now.